Insurance Claims
HIPAAtherapy can send insurance claims on your behalf and track whether the payer accepted them for processing. The feature is in beta. This page covers what’s live today, how the workflow runs, and what still needs to happen outside the app.
What’s in scope today
Section titled “What’s in scope today”HIPAAtherapy currently supports:
- Eligibility checks - confirm a client’s coverage and benefits before the session
- Claim submission - send professional insurance claims (837P files) to the payer through Stedi (our insurance clearinghouse partner)
- Acknowledgment tracking - receive claim status responses through Stedi and surface accepted or rejected status on the claim
- Rejected claim correction and refile - fix a rejected claim and refile it as a fresh submission
- Replace and void - once the payer confirms a claim with a control number, send a corrected version or void the claim entirely
What HIPAAtherapy does not do yet is covered under current limitations.
How a claim moves through HIPAAtherapy
Section titled “How a claim moves through HIPAAtherapy”- You check eligibility for the client’s insurance
- You fill in diagnosis codes, place of service, and the services being billed (service lines) on the session, then submit
- HIPAAtherapy sends the claim through Stedi
- Stedi forwards the claim to the payer
- The payer sends back an acknowledgment, and the claim moves to Accepted or Rejected in HIPAAtherapy
HIPAAtherapy checks for new acknowledgments every 15 minutes.
Before you submit a claim
Section titled “Before you submit a claim”A few pieces of data have to be in place before you can submit a claim.
Practice settings (Settings > Practice):
- NPI
- EIN
- Office phone
- Taxonomy code
- Office address, including zip code
Staff profile (My Profile):
- Taxonomy code (rendering provider)
- NPI, if the rendering provider uses a different NPI from the practice
Client record:
- Date of birth and a current address
- At least one insurance on file, with member ID and - when the plan uses them - group and policy numbers
If any of the practice settings are missing, the session page shows a notice and hides the Submit Claim button until you complete them.

Checking eligibility
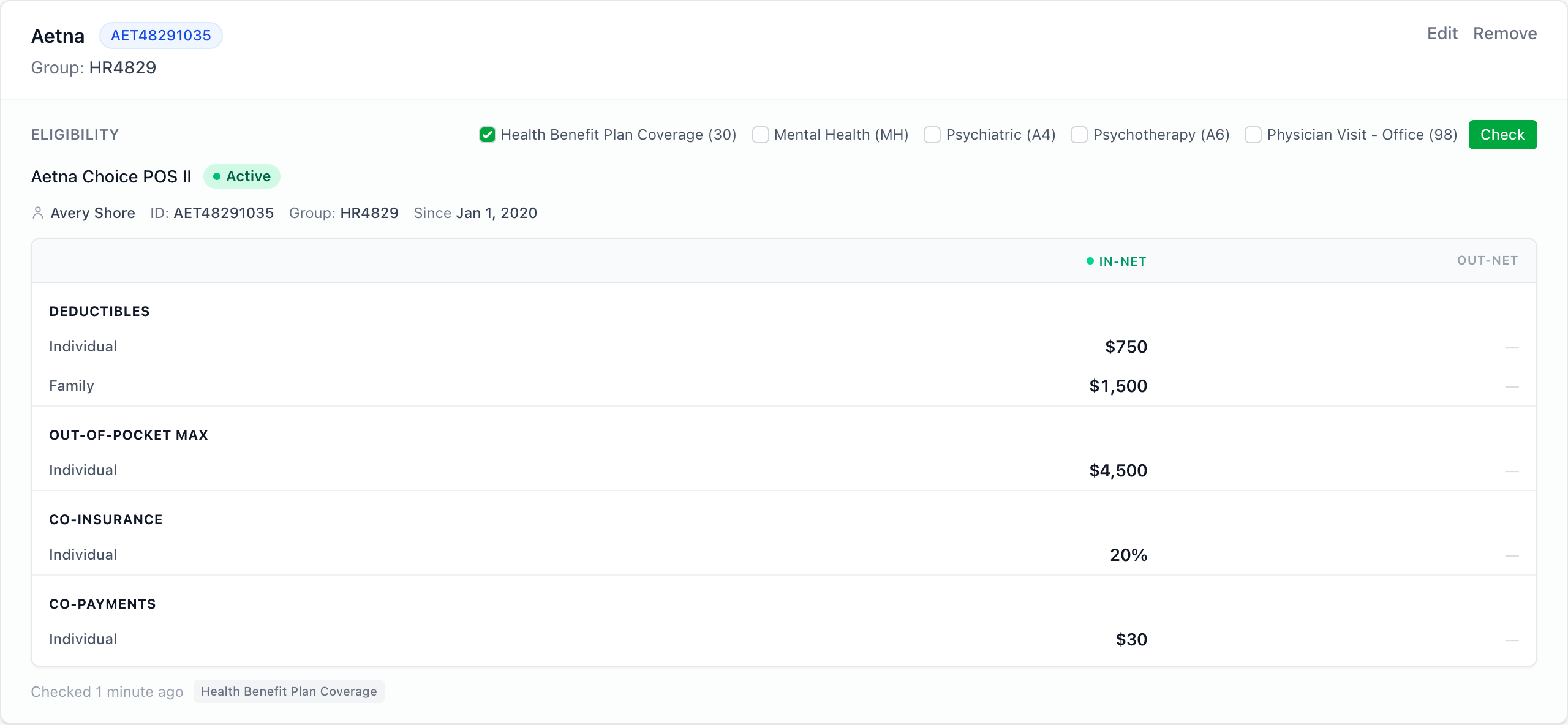
Section titled “Checking eligibility”- Open the client’s profile
- Go to the Insurance section and select the plan you want to check
- Click Check
- Benefits, co-pay, deductible, and plan status usually appear within a few seconds
Submitting a claim
Section titled “Submitting a claim”From a session page, scroll to the Insurance Claim section.
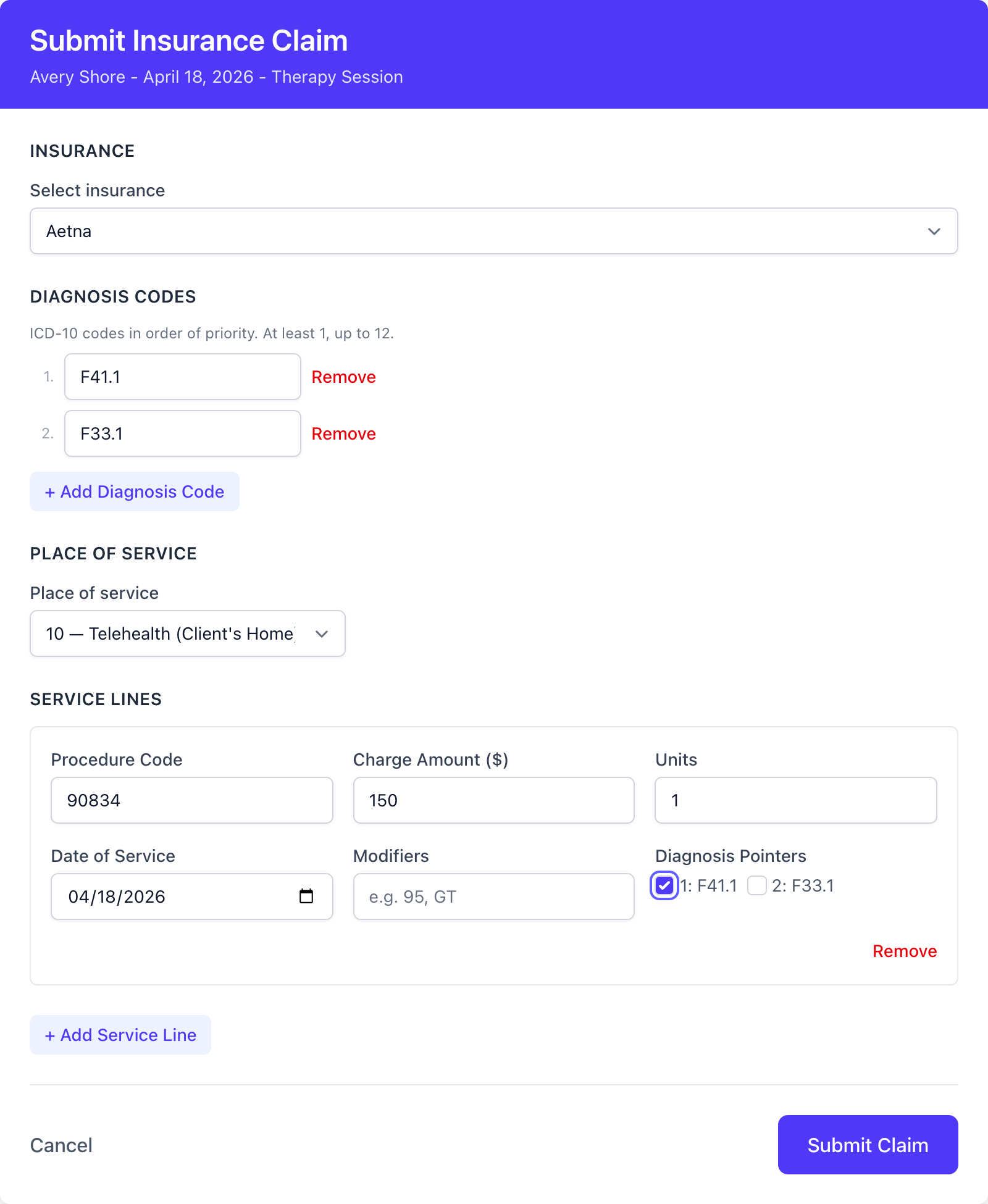
- Click Submit Claim
- Pick the insurance, diagnosis codes (up to 12, in priority order), place of service, and one or more service lines. Each service line lists the procedure code, charge, units, date of service, any modifiers, and which diagnosis the service is tied to
- Click Submit Claim at the bottom of the form
The claim moves through these states:
| State | What it means |
|---|---|
| Pending | The claim has been queued but hasn’t been transmitted yet |
| Submitted | Stedi accepted the claim; the payer hasn’t responded yet |
| Accepted | The payer sent a claim acknowledgment (277CA) indicating the claim was accepted for processing |
| Rejected | Stedi or the payer rejected the claim |
| Failed | The submission didn’t complete - transmission timed out or HIPAAtherapy hit an error before sending |
“Accepted for payer processing” doesn’t mean the claim has been paid. It means the payer accepted the claim into its processing workflow. Final payment, denial, and adjustment details arrive on a separate payment report (the 835 ERA), which isn’t supported yet.
Payers not available for claim submission yet
Section titled “Payers not available for claim submission yet”Most supported payers accept claims as soon as your practice’s billing details are in place. A small portion don’t - some require a one-time enrollment between your practice and the payer first, and a few don’t yet support electronic claim submission through Stedi at all. For that subset, the claim form shows a warning when you pick the insurance:
Claim submission isn’t available for this payer yet. Eligibility checks still work.
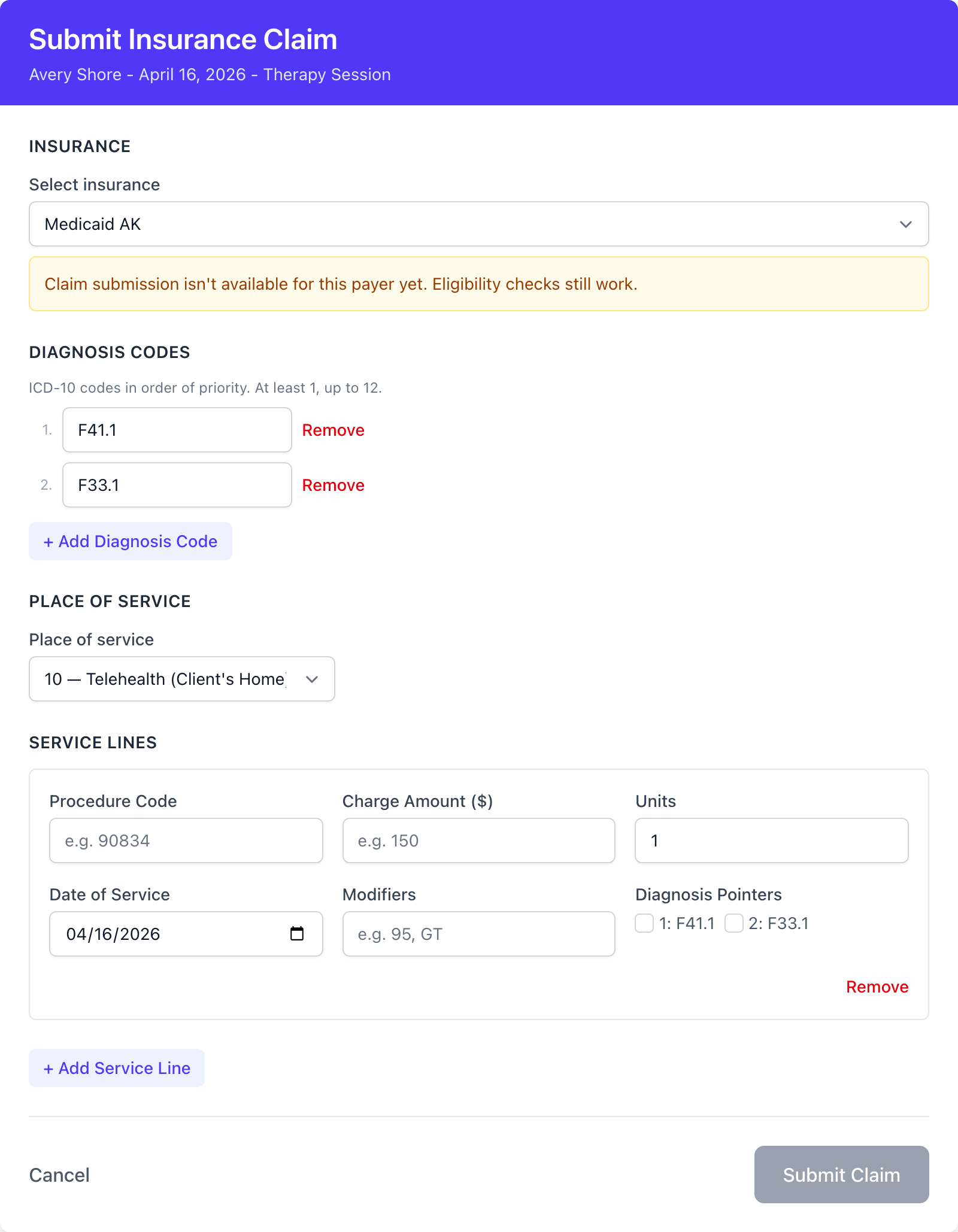
Eligibility checks keep working for these payers in the meantime. We’re actively building in-app support for payer enrollment, which will cover the enrollment-required case - see Current limitations.
Reading the claim status
Section titled “Reading the claim status”Every claim lives on its session. Open the session and look at the Insurance Claim section to see:
- The current status and when the acknowledgment arrived
- The rejection message from Stedi or the payer (on rejections)
- The claim details that were transmitted (diagnosis codes, service lines, payer)
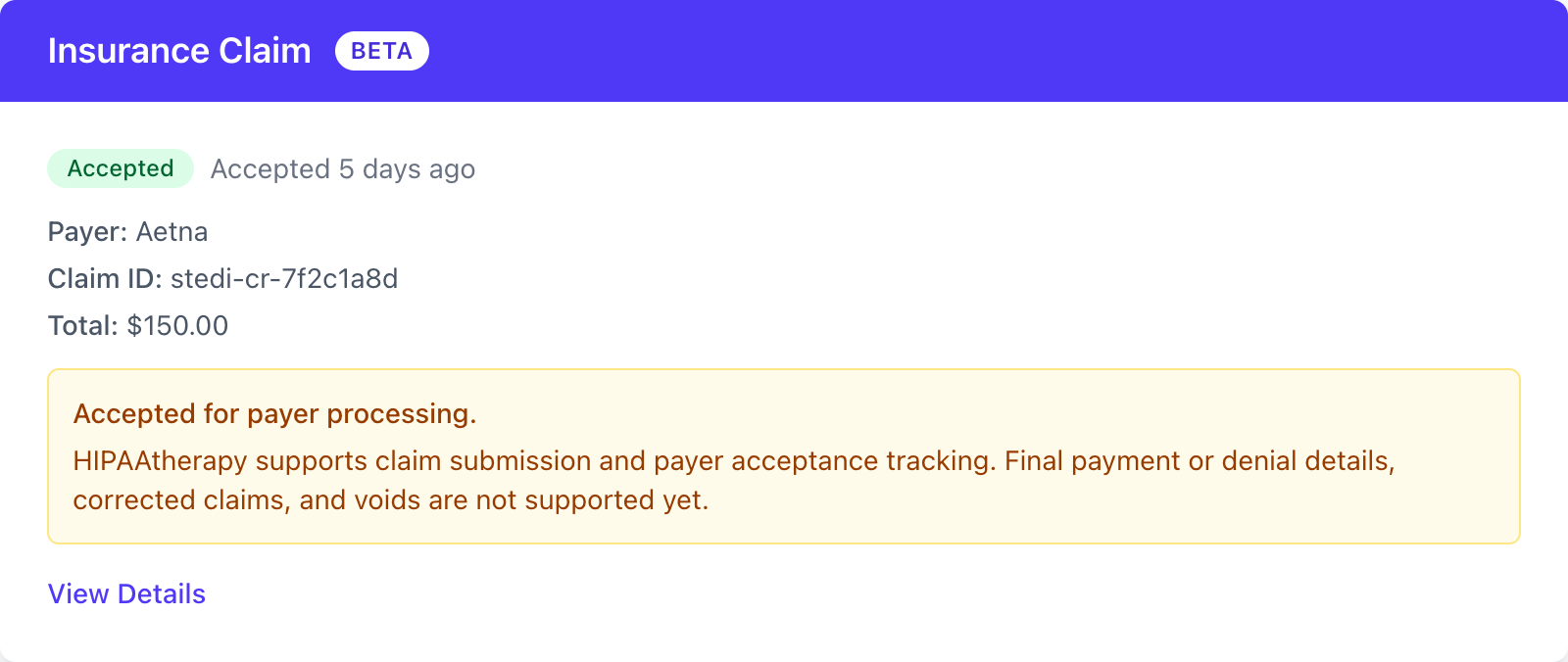
Accepted claims
Section titled “Accepted claims”An accepted claim has entered the payer’s review process. Once the payer also returns a claim number, the claim becomes eligible for in-app corrections - see Correcting an accepted claim below.
Payment and denial details aren’t available in HIPAAtherapy yet, so reconcile the actual payment from your payer portal or EOB for now. In-app payment posting is planned.
Rejected claims
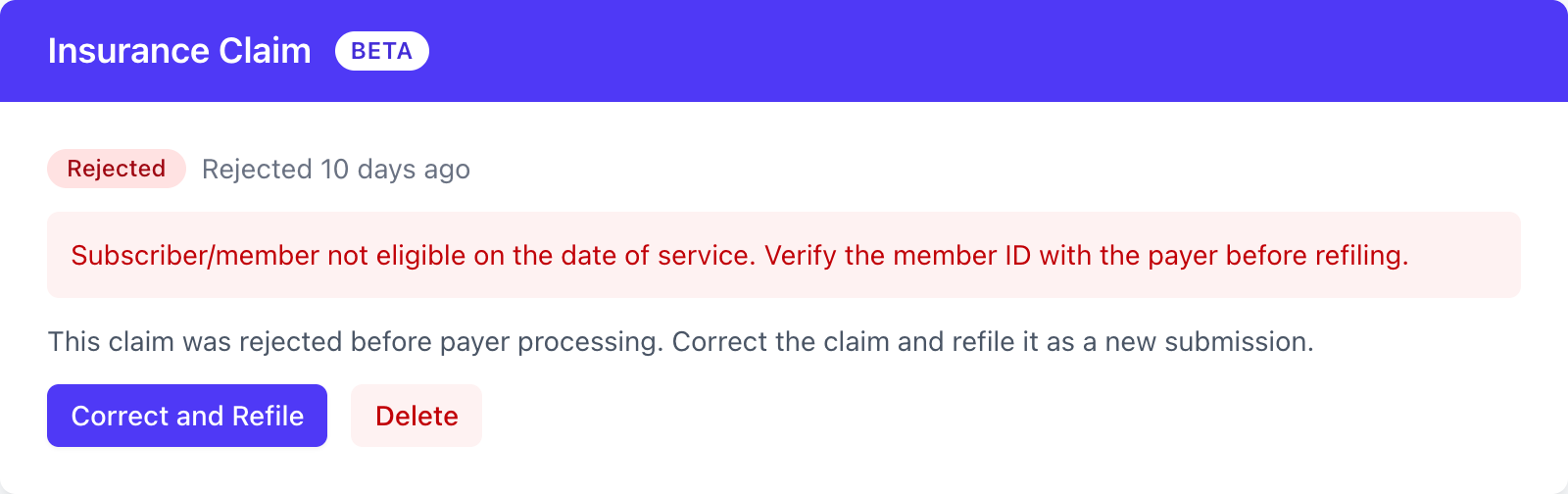
Section titled “Rejected claims”A rejection can come from two places: Stedi (the claim failed Stedi’s claim validation checks - called claim edits - so the payer never saw it) or the payer (the payer received the claim but won’t put it through review). Typical payer rejections: an invalid NPI, a member ID that doesn’t match the payer’s records, or a mismatch between a service and the diagnosis it’s tied to. Either way, the rejection message is shown on the claim.
To resolve a rejected claim, use the actions on the claim section:
- Correct and Refile - opens a fresh claim form for the same session. Make your corrections and submit.
- Delete - removes the rejected claim if you don’t want to refile.
Correcting an accepted claim
Section titled “Correcting an accepted claim”Once a claim is accepted, you can correct it in two ways: Replace to send a corrected version, or Void to cancel the claim with the payer.
Both depend on the payer returning a payer claim number (also called a payer control number, or PCCN). This is the payer’s own identifier for the claim - they need it on the corrected or void submission to tie it back to the original. The payer claim number arrives on the acknowledgment from the payer; until then, Replace and Void stay disabled with a “Waiting for … to confirm processing” note on the claim.
Replace a claim
Section titled “Replace a claim”Use Replace when the original claim was accepted but had something wrong - a procedure code mismatch, a missing modifier, the wrong diagnosis tied to a service. The replacement supersedes the original with the payer.
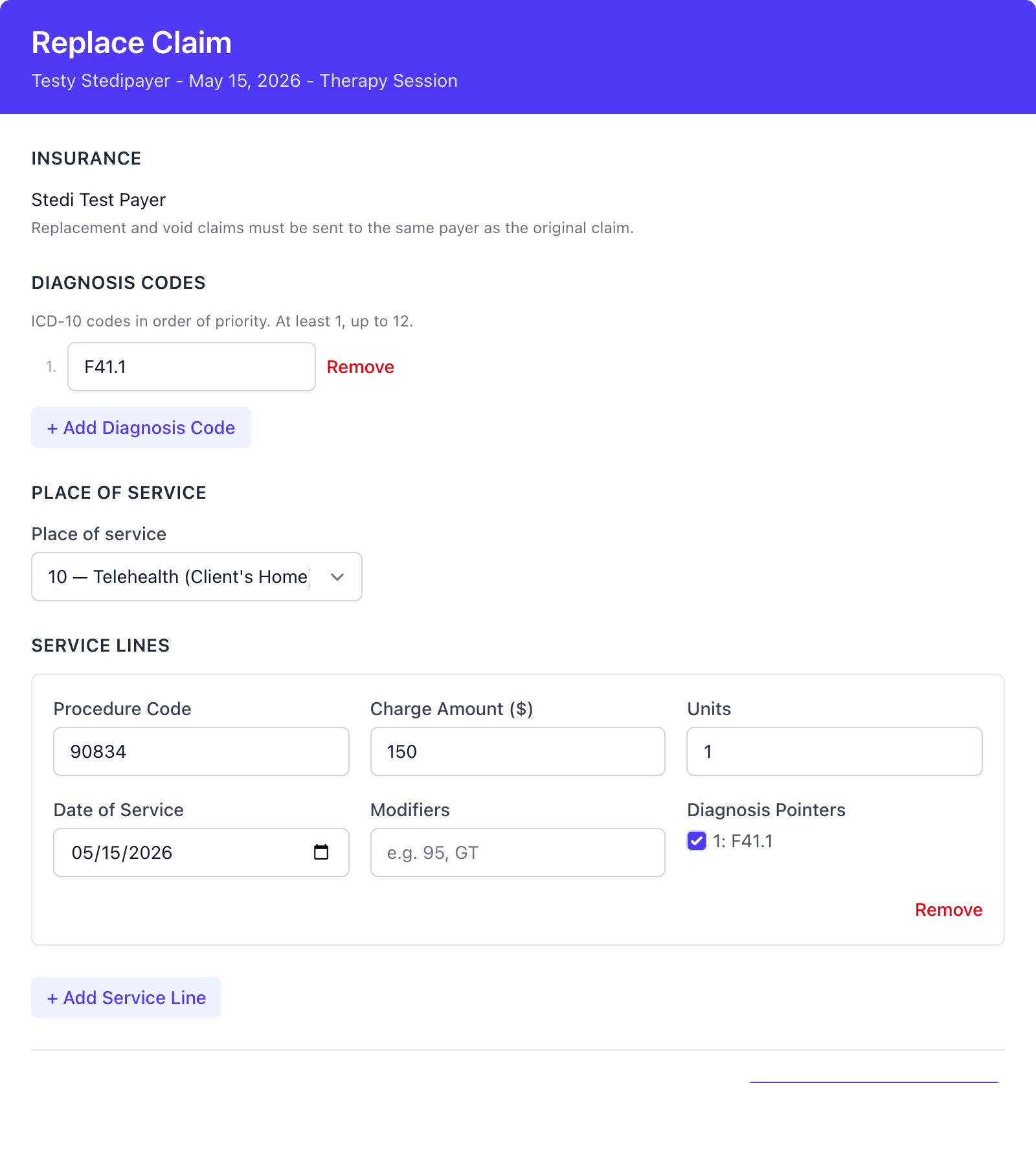
- From the session, find the accepted claim and click Replace
- The form pre-fills with the original claim’s details. The insurance is locked - replacements have to go to the same payer as the original
- Make your edits and click Submit Replacement
The replacement goes through the same submit and acknowledgment cycle as an initial claim. If the payer accepts the replacement, it becomes the current version of the claim for that session.
Void a claim
Section titled “Void a claim”Use Void to retract a claim entirely - typically when you billed the wrong session, the wrong client, or shouldn’t have billed at all. There’s no edit form: HIPAAtherapy sends a void transaction referencing the payer claim number.
Click Void on the accepted claim and confirm. Once the payer acknowledges the void, the claim and any of its replacements are closed and the session shows:
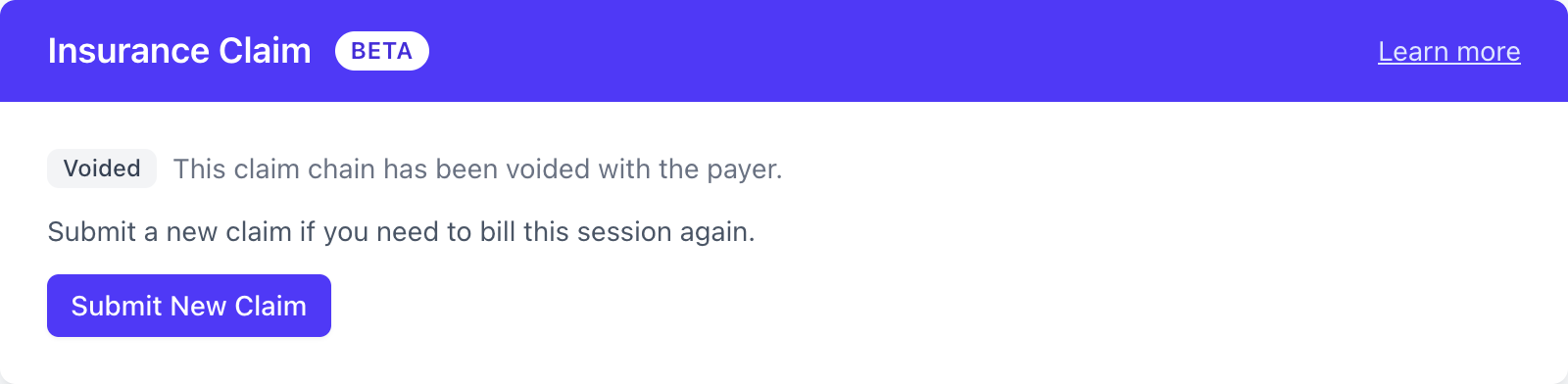
If you need to bill the session after voiding, use Submit New Claim to start over.
When Replace and Void aren’t available
Section titled “When Replace and Void aren’t available”A few cases where these actions won’t show up or stay disabled:
- No payer claim number yet. Wait for the payer to confirm processing. The claim section shows a “Waiting for …” note while we wait.
- Payer doesn’t support that action. Original Medicare handles replacements differently and doesn’t support void at all. The claim section says which action isn’t supported.
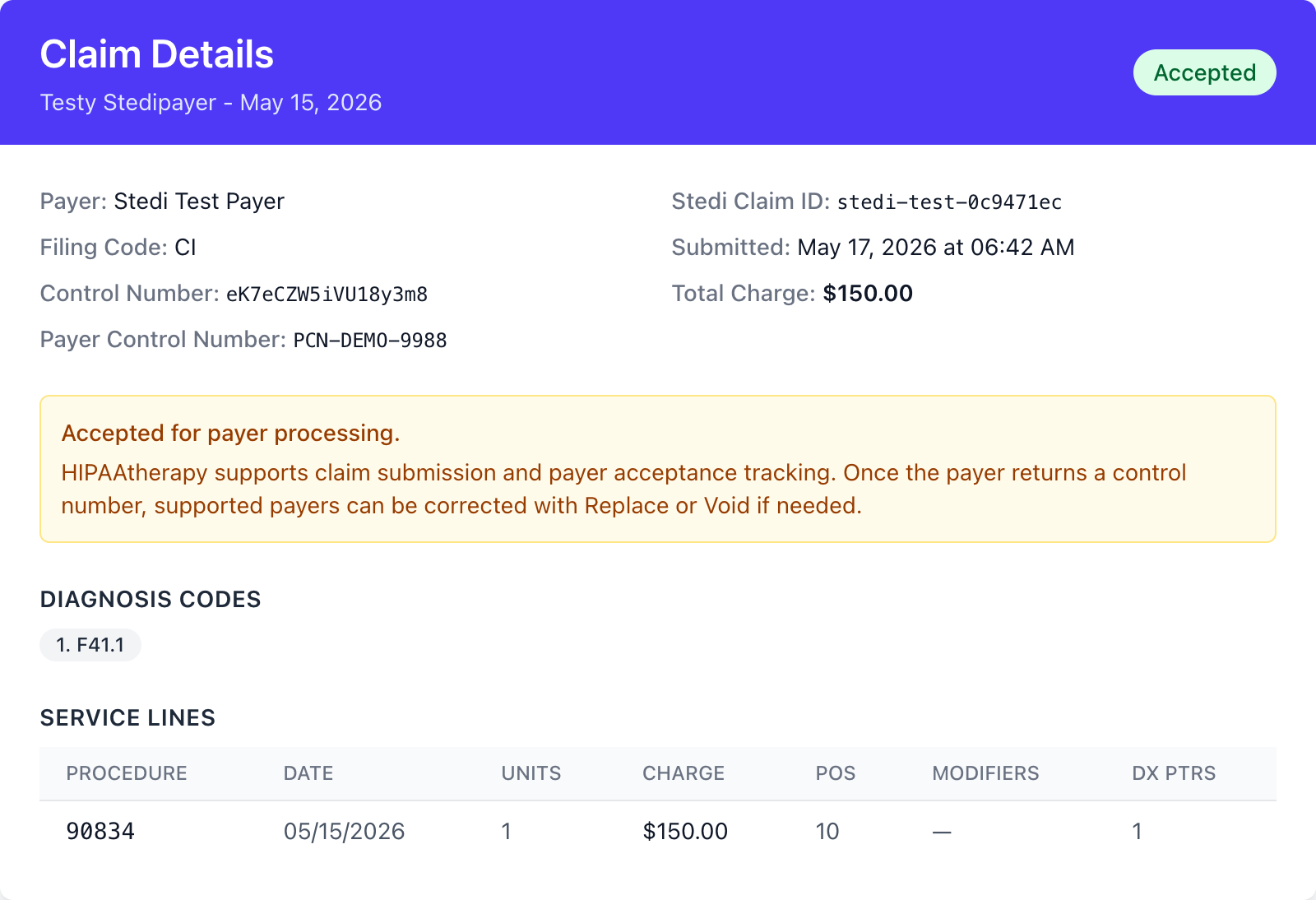
Reading claim details
Section titled “Reading claim details”The claim Details page shows the identifiers for the current claim - HIPAAtherapy’s claim tracking number, the payer claim number (once it arrives), the Stedi claim ID, and the Intent (Replacement or Void) for any non-initial claim.
Current limitations
Section titled “Current limitations”The insurance feature is rolling out in phases. Here’s what’s not supported yet, so you can plan around it.
Payment posting
Section titled “Payment posting”Final payment, client responsibility, adjustments, and denials all arrive on the payment report (the 835 ERA). HIPAAtherapy doesn’t ingest the 835 yet. Once a claim is accepted, reconcile payment from your payer portal or EOB.
Correcting a claim after the payer reviews it
Section titled “Correcting a claim after the payer reviews it”If the payer denies a claim during its review, the denial arrives on the 835 ERA - which we don’t ingest yet. Replace and Void work off the acceptance acknowledgment, not the denial report, so corrections after the payer’s review still need to be handled in your payer portal for now.
Self-service payer enrollment
Section titled “Self-service payer enrollment”Some payers require a one-time enrollment before they’ll accept claims from your practice. HIPAAtherapy currently shows a warning on the claim form for these payers but doesn’t yet provide a way to complete the enrollment in-app. Until the in-app enrollment flow is available, those payers are blocked for claim submission inside HIPAAtherapy.
Frequently asked questions
Section titled “Frequently asked questions”Does “Accepted” mean I’ve been paid? No. Accepted means the payer has queued the claim for review. HIPAAtherapy doesn’t post payment information yet, so reconcile payments from your payer portal or EOB for now. In-app payment posting is planned.
Can I resubmit a rejected claim? Yes. Correct and Refile opens a fresh claim form for the same session. If the form refuses to submit because the previous rejected claim is still blocking a new submission, Delete the rejected claim first and then refile.
What if I pick the wrong insurance at submission? If the claim is rejected or failed, delete it and file a new one. If it’s pending or submitted, there isn’t an in-app cancel or edit path yet. If it’s already accepted and you’ve billed the wrong insurance entirely, use Void to cancel it with the payer, then submit a new claim against the correct insurance.
What’s the difference between Replace and Void? Replace sends a corrected version of the claim - same session, same payer, with your edits. Void cancels the claim entirely. Both need the payer to have returned a payer claim number first.
Can I still bill clients directly while this is in beta? Yes. Claim submission is optional per session. Cash, card, and invoice flows work independently of the insurance workflow. See Payments for details.
Why is the feature in beta? Because parts of the end-to-end billing workflow - payment posting, corrections after the payer’s review, self-service enrollment - are still being built. Submission, acknowledgment, replace, and void are stable, but you should plan on doing payment reconciliation outside the app for now.